|
 |
- Search
| Epilia: Epilepsy Commu > Volume 3(2); 2021 > Article |
|
Abstract
Table 1.
Scores on this revised stigma scale range from 0 to 9, with a score of 0 indicating that the person does not feel stigmatized, scores of 1–6 indicating that the person feels mildly to moderately stigmatized, and scores of 7–9 indicating that the person feels highly stigmatized.11
In the original version, individuals are asked to respond on a yes/no scale. Therefore, scores range from 0 to 3, where a score of 0 indicates that the person does not feel stigmatized and a score from 1 to 3 indicates that the person does feel stigmatized. The higher the score, the greater the person’s perception of stigma.9
Table 2.
| Study | Year | Design | Participants | Measure | Definition of stigma | Prevalence of felt stigma | Analysis | Associated factor |
|---|---|---|---|---|---|---|---|---|
| Lee et al.8 | 2005 | Cross-sectional | Adults with chronic epilepsy (n = 400) | SSE-3 | Score ≥ 1 | 0.31 | Multiple logistic regression | Enacted stigma, introverted personality, problem solving controllability, emotional subscale of QOLIE-31 |
| Ryu et al.20 | 2015 | Cross-sectional | Adolescents with chronic epilepsy and their mothers (n = 243 pairs) | CSS, PSS | - | - | Multiple linear regression | Higher maternal concealment behavior, adolescents’ lower level of epilepsy knowledge, receiving antiepileptic polytherapy |
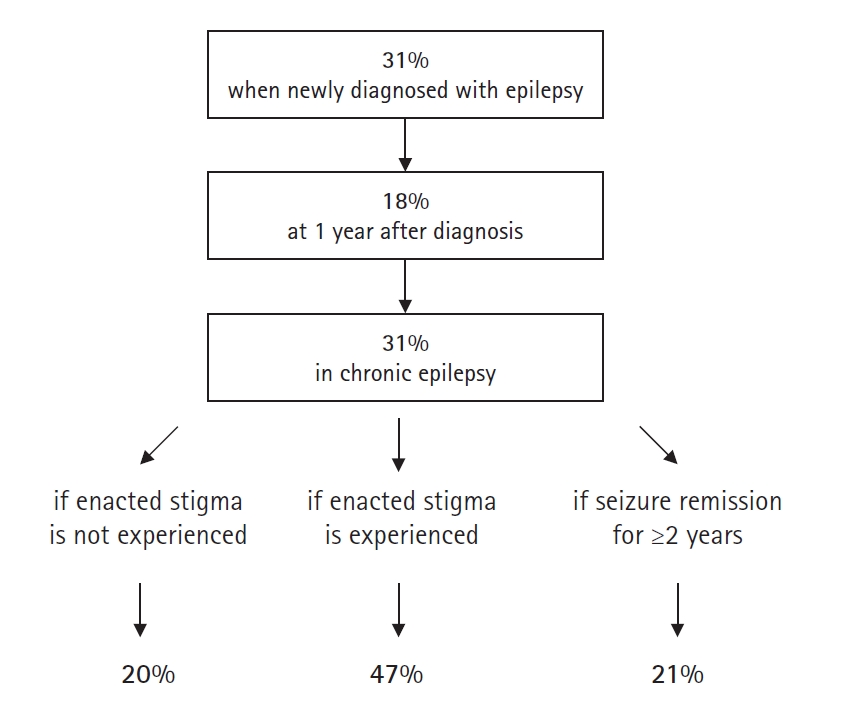
| Lee et al.13 | 2016 | One-year longitudinal | Adults with newly diagnosed epilepsy (n = 218 at baseline; n = 153 at 1-year follow-up) | SSE-3 | Score ≥ 1 | 31% at the time of diagnosis; 18% at 1 year after diagnosis | Multiple logistic regression | Introverted personality and a high level of anxiety for felt stigma at the time of diagnosis; introverted personality and lower economic status for felt stigma at the 1-year follow-up |
| Lee et al.17 | 2020 | Cross-sectional | Family members of persons with epilepsy (n = 482) | SSE-3R | Score ≥ 1 and | 54% by score ≥1 and 10% by score ≥4 | Stepwise logistic regression | High seizure frequency, being a sibling or offspring of a patient |
| score ≥ 4 | ||||||||
| Lee et al.15 | 2021 | Cross-sectional | Seizure-free adults for ≥2 years (n = 81) | SSE-3 | Score ≥ 1 | 0.21 | Stepwise logistic regression | Enacted stigma, neurotic personality |
Table 3.
| Study | Year | Design | Participant | Main outcome | Measure | Analysis | Finding |
|---|---|---|---|---|---|---|---|
| Han et al.21 | 2015 | Cross-sectional | Adults with chronic epilepsy and their caregivers (n = 391 pairs) | Depression | BDI, SSE-3, CBI | Hierarchical linear regression | Patients’ BDI scores were significantly associated with employment status, GTC seizure frequency, polypharmacy, patients’ felt stigma, and caregivers’ BDI scores. Caregivers’ felt stigma was indirectly associated with patients’ BDI scores through caregivers’ depression. |
| Seo et al.25 | 2015 | Cross-sectional | Adults with chronic epilepsy (n = 266) and controls (n = 170) | Aggression | AQ, SSE-3R, NDDI-E, GAD-7 | Stepwise linear regression | PWEs had higher overall AQ scores and anger and hostility subscale scores than controls. The strongest predictor for the overall AQ score was the SSE-3R score, followed by the GAD-7 score, and the NDDI-E score. |
| Lee et al.26 | 2017 | Cross-sectional | Seizure-free adults for ≥1 years (n = 225) | Concealment of epilepsy diagnosis | DMS, SSE-3, HADS | Multiple linear regression | 76% stated that they often or sometimes kept their epilepsy a secret. Felt stigma was identified as the only independent factor associated with DMS scores (P = 0.031), while HADS depression lost significance (P = 0.057). |
| Han et al.22 | 2019 | Cross-sectional | Adults with chronic epilepsy (n = 219) | Social anxiety | SPS-6, SIAS-6, SSE-3R, PHQ-9, DMS, F-APGAR | Multiple logistic regression | SPS-6 scores ≥9 were independently associated with SSE-3R scores of 4–9 (OR, 8.626), SSE-3R scores 1–3 (OR, 5.496), and PHQ-9 scores ≥10 (OR, 4.092). In contrast, SIAS-6 scores ≥12 were related only to PHQ-9 scores ≥10 (OR, 8.740). Epilepsy-related variables were not related to social anxiety. |
| Lee et al.24 | 2020 | Cross-sectional | Adults with chronic epilepsy (n = 312) | Health-related quality of life | QOLIE-10, SSE-3, ESES, HADS | Stepwise linear regression, analysis of covariance | QOLIE-10 scores were positively correlated with ESES score and employed status, but negatively correlated with HADS scores, felt stigma, seizure frequency, and polytherapy. Self-efficacy correlated with QOLIE-10 scores only in subjects with recurrent seizures and in those with felt stigma. |
| Lee et al.23 | 2021 | Cross-sectional | Adults with chronic epilepsy (n = 357) | Health-related quality of life | QOLIE-31, SSE-3, HADS, RSES, EPQ-RS | Hierarchical linear regression | QOLIE-31 scores were significantly associated with being married, polypharmacy, neuroticism, depression, anxiety, self-esteem, and felt stigma. |
| Lee et al.15 | 2021 | Cross-sectional | Seizure-free adults for ≥2 years (n = 81) | Health-related quality of life | QOLIE-31, SSE-3, HADS, RSES, EPQ-RS | Stepwise logistic regression, Sobel test | Felt stigma was not associated with the total QOLIE-31 scores. Felt stigma had indirect effects on the QOLIE-31 scores through EPQ-RS neuroticism scores, but its statistical significance was lost after controlling for the presence of enacted stigma, anxiety, and depressive symptoms. |
BDI, Beck Depression Inventory; SSE-3, Three-item Stigma Scale for Epilepsy; CBI, Caregiver Burden Inventory; GTC, generalized tonic-clonic; AQ, Aggression Questionnaire; SSE-3R, SSE-3 Revised; NDDI-E, Neurological Disorders Depression Inventory for Epilepsy; GAD-7, Generalized Anxiety Disorder-7; DMS, Disclosure Management Scale; HADS, Hospital Anxiety Depression Scale; SPS-6, Social Phobia Scale; SIAS-6, Social Interaction Anxiety Scale; PHQ-9, Patient Health Questionnaire-9; F-APGAR, Family Adaptation, Partnership, Growth, Affection, Resolve; OR, odds ratio; QOLIE, Quality of Life in Epilepsy; ESES, Epilepsy Self-Efficacy Scale; RSES, Rosenberg Self-esteem Scale; EPQ-RS, short form of the Eysenck Personality Questionnaire-Revised.
References
-
METRICS

-
- 0 Crossref
- 2,335 View
- 44 Download
- Related articles in Epilia: Epilepsy Commun
-
Vagus Nerve Stimulation for Patients with Epilepsy2021 September;3(2)
Physical Exercise in Patients with Epilepsy2021 March;3(1)
Contraception for Women with Epilepsy2020 September;2(2)
Prospects of Seizure Prediction Technology for Patients with Epilepsy2020 September;2(2)
Characteristics and Medical Treatment of Elderly Patients with Epilepsy 2020 September;2(2)